Welcome to your go-to guide for the low FODMAP diet. This complete guide will teach you the fundamentals of the low FODMAP diet and get you started on the first phase, also known as the low FODMAP elimination phase.
This article will cover:
- Safety tips: what to do before you start
- Who should use the low FODMAP diet?
- What is the low FODMAP diet? Overview of the three phases
- What are FODMAPs?
- How do FODMAPs trigger symptoms?
- Tips for starting the low FODMAP diet
- Making The Diet Easy: Your FODMAP Guide
- Are A Little Bit Yummy recipes suitable for the first phase?
- Common FODMAP diet questions
- When do you start the reintroduction phase?
Safety Tip: Before you get started
Before starting the low FODMAP diet, you need to talk to your doctor to check if the diet is right for you.
Your doctor needs to rule out that your gut symptoms are not being caused by other conditions like coeliac (celiac) disease, inflammatory bowel disease, Crohn’s disease, or cancer (1 2). Unlike Irritable Bowel Syndrome (IBS), these medical conditions cause damage to the gut, and require different treatment plans. Once you are on the low FODMAP diet, testing for some of these medical conditions can become more challenging.
Who should use the low FODMAP diet?
The low FODMAP diet is predominantly used to help people with IBS reduce their gut symptoms and identify their food triggers. Research shows that the low FODMAP diet can help up to 75% of people with IBS improve their symptom management and reduce bloating, distension, excess gas and altered bowel movements (diarrhoea and constipation) (3).
What is the low FODMAP diet?
Essentially the low FODMAP diet is a medical diet that can help you manage your gut symptoms and learn about your food triggers. It’s best to think of this diet as a learning journey that has three phases:

1. Low FODMAP Phase or Elimination Phase:
The goal is to reduce the amount of FODMAPs you eat by focusing on low FODMAP foods and serving sizes. The goal is to see if FODMAPs are affecting your gut symptoms. This phase only lasts for 2 to 6 weeks.
2. FODMAP Reintroduction Phase:
In this phase, you complete a series of food challenges using specific high FODMAP foods to see which of the FODMAP groups affect your gut. This phase is sometimes called the Challenge phase.

3. Adapted FODMAP Diet or Personalisation Phase:
You relax your strict low FODMAP diet by bringing back the FODMAP groups you tolerated well during the reintroduction phase. This process helps keep your gut symptoms calm while improving your food variety and making socialising/eating out much easier.
It’s important to note that the low FODMAP phase is not a permanent way of eating and should only be followed strictly for 2 to 6 weeks before moving into the FODMAP reintroduction phase (4,5). In addition, this medical diet can be complex to navigate, so it should be followed with the help of guided support and an experienced FODMAP trained dietitian.
What are FODMAPs?
Now we are getting into the nitty-gritty of the diet. If you are sitting there thinking FOD-what? you aren’t the only one. In super simple terms, FODMAPs are fermentable short-chain carbohydrates, aka naturally occurring sugars (don’t worry, the diet isn’t sugar free). FODMAPs occur in a wide range of fruit, vegetables, cereals, grains, dairy products, legumes and pulses. The goal of the low FODMAP phase is not to cut out entire food groups but to reduce your FODMAP intake by reducing your portion sizes and switching out certain high FODMAP foods.
Let’s start by breaking down the FODMAP acronym:
F
O
Oligosaccharides
We can break this complex-sounding FODMAP group into two subgroups: fructans and galactans. Fructans (fructo-oligosaccharides or FOS) are found in foods like onion, garlic, wheat, rye, barley and dried fruit. Galactans (galacto-oligosaccharides or GOS) can be found in foods like silken tofu, pistachios, cashews, legumes and pulses (5 6).
Have you ever wondered why beans make people fart? This excess gas happens because humans weren’t born with the enzymes needed to digest oligosaccharides, so they will make everyone gassy but only trigger gut-based symptoms in some people with sensitive guts (2 6).
D
Disaccharides
The only disaccharide you need to worry about is lactose which is found in some products made from cow, sheep or goat’s milk. Lactose contains two sugar units that need to be ‘unzipped’ using an enzyme called lactase before our bodies can absorb it. If your gut lacks lactase enzymes, then you will struggle to process high lactose products and the lactose might trigger symptoms.
Lactose is found in milk, yoghurt and products like sour cream or cream cheese (5 6). The good news is that hard cheeses, lactose free milk or yoghurt, and butter are all okay when you are on the low FODMAP diet.
M
Monosaccharides
Here we are talking about excess fructose – which is when there is more fructose than glucose in a food. Our bodies need an equal amount of glucose in the food to help the fructose be absorbed in the small intestine (2 6). When you are on the low FODMAP diet, we only need to restrict foods containing excess fructose like apples, pears, mango, lychee, asparagus, honey and high fructose corn syrup.
A P
And Polyols
Polyols are sugar alcohols, but they won’t make you drunk. This FODMAP group is broken down into two subgroups: mannitol and sorbitol. These sugar alcohols are found in a wide range of fruit (like apples, pears, stone fruit) and vegetables (like mushrooms and celery). They can also be artificially made and used as low-calorie artificial sweeteners. Make sure you check products like protein powders, chewing gum, diabetic candy and low sugar/sugar free products for these sweeteners.
The reason polyols can be problematic for some people is because they are only partially absorbed in our small intestines. The remaining polyols continue to our large intestine, where they are fermented by our gut bacteria (2 6).
How do FODMAPs trigger symptoms?
So you now know what FODMAPs are, but how do they trigger symptoms?
When you eat FODMAPs they travel through your stomach and into your small intestine. Here, they are poorly absorbed and draw water into our bowel. Next, the FODMAPs travel to our large intestine, where our gut bacteria ferment them as they break down the food. This fermentation can create gas that can trigger gut-based symptoms like excess wind, bloating, distension, diarrhoea, and constipation when combined with the excess water.
How long should you stay on a low FODMAP diet?
A strict low FODMAP diet is not for life. The diet’s first phase, where you reduce your FODMAP intake, should only last for 2 to 6 weeks. Once you see if the low FODMAP diet helps significantly reduce your gut symptoms, it’s time to move on to the FODMAP reintroduction phase.
High FODMAP foods can be important for long-term gut health, so it’s important to bring some high FODMAP foods that don’t trigger symptoms back into your diet.
Tips To Help Get You Started
If you’ve decided it’s time to start transitioning onto the low FODMAP diet. Just remember you don’t have to do this all at once; we often find people do better if they transition onto the diet over a couple of weeks.
Here are some quick tips to get you started:
1. Keep a record of your symptoms. Write down what your symptoms have been like over the past week. These symptom notes will help you track your progress and see if the diet is working. Our online symptom tracker can also make this process easy when you join the FODMAP Made Easy program.
2. Find an up-to-date high FODMAP and low FODMAP food list. Online lists and free FODMAP apps go out of date every few months, so we recommend using the Monash University FODMAP Diet App or our food lists in our FODMAP Made Easy program.
3. Write down what you plan to eat over the next four days and start by swapping out high FODMAP foods you eat regularly for low FODMAP options using a food list.
4. Check your processed foods for sneaky high FODMAP ingredients. This label reading guide can help.
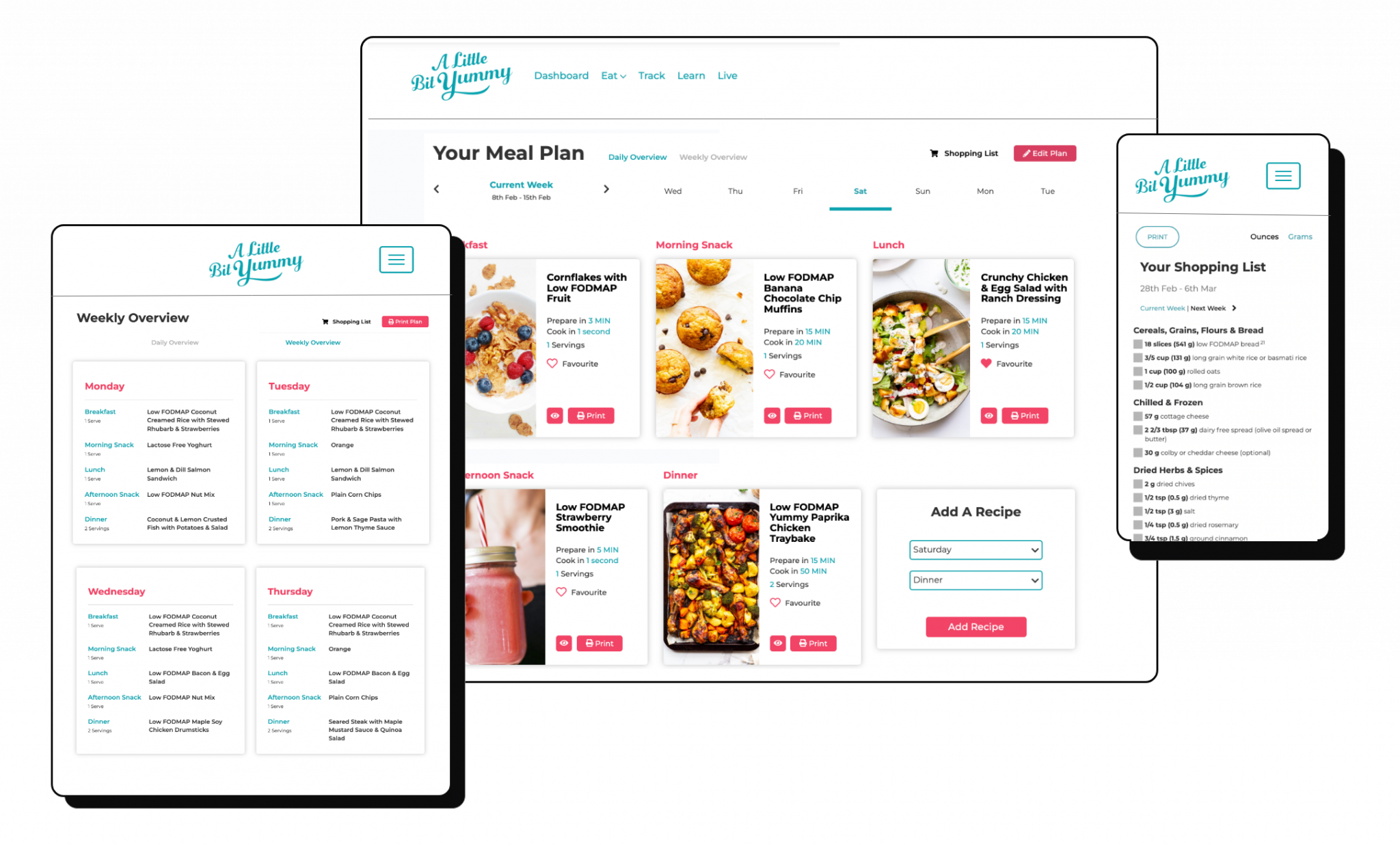
5. Create a low FODMAP meal plan. It would help if you had a couple of breakfast ideas, 4 or 5 snack ideas (including a treat), 2 to 3 easy lunch ideas and 5 low FODMAP dinner ideas to get you started. We’ve got over 1200+ low FODMAP recipes and meal planning tools to help get you started in our FODMAP Made Easy program.
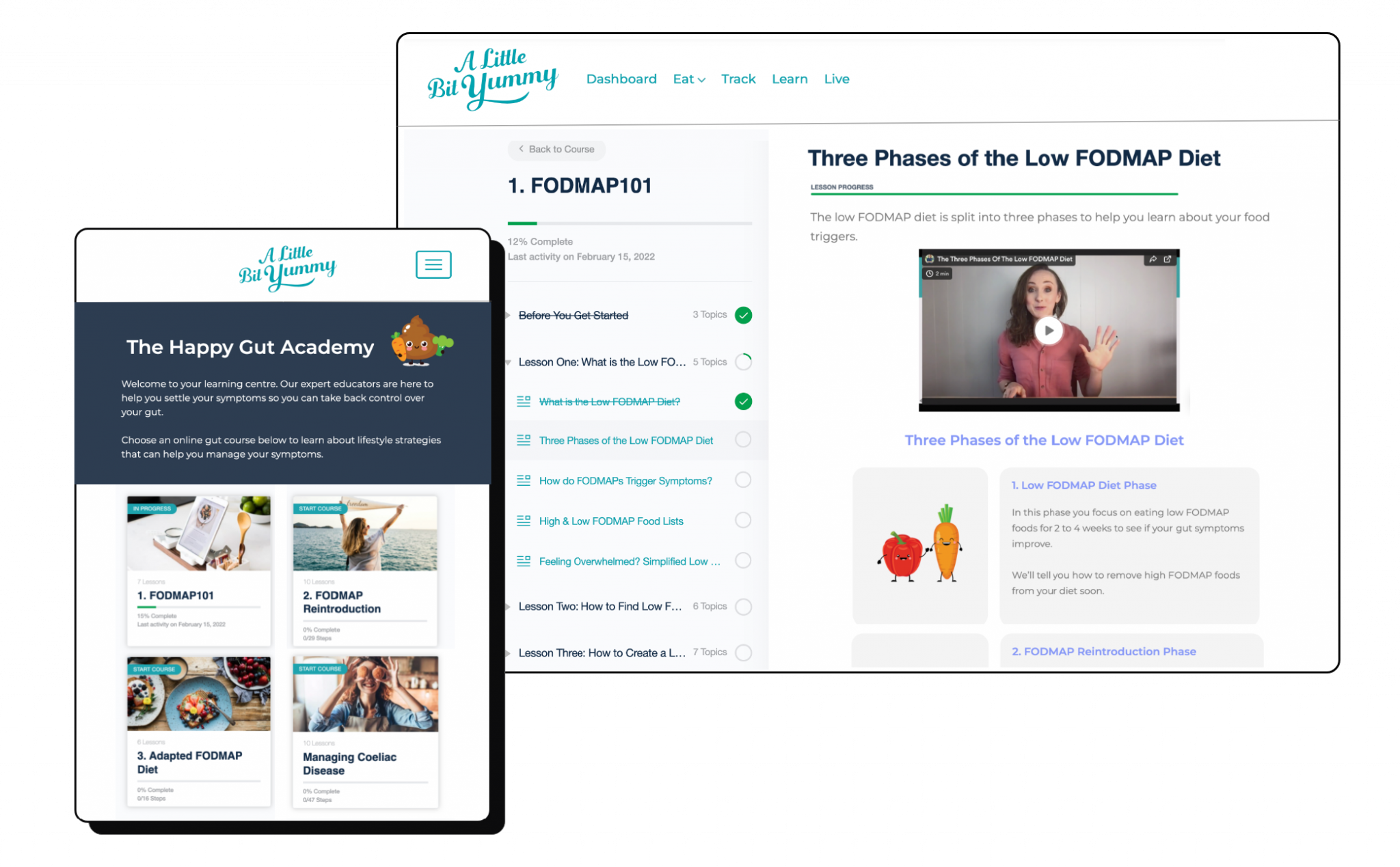
FODMAP Made Easy
It’s okay if moving onto the low FODMAP diet feels hard. We are here to help make things easy. Our FODMAP Made Easy program has EVERYTHING you need to settle your symptoms and identify your trigger foods.
We’ll guide you through the three phases of the low FODMAP diet with online courses, delicious recipes, helpful handouts, meal planning tools, weekly support emails and dietitian-led classes. You can also email our FODMAP team for extra help.
When it’s time to find your food triggers we’ll help you manage your anxiety and give you step-by-step instructions on how to reintroduce each of the FODMAP groups.
Are A Little Bit Yummy recipes suitable for the first phase?
Yes, they are! Our recipes are made using the low FODMAP guidelines from Monash University (the lead researchers of the low FODMAP diet). Each recipe is also checked by a FODMAP trained registered dietitian so you can eat with confidence. These checks mean you can use our recipes during the low FODMAP phase. We also regularly update our recipes as low FODMAP recommendations change.
Are portion sizes important in the low FODMAP diet?
They sure are! Foods often have low FODMAP, moderate FODMAP and high FODMAP portion sizes, so understanding portion sizes can help you reduce your FODMAP load faster. The goal is to focus on eating low FODMAP portion sizes during the first phase of the diet. We talk about portion sizes more here.
Is the low FODMAP diet gluten free?
The short answer is no. Gluten isn’t high FODMAP – it’s the oligosaccharides in wheat, rye and barley that can be a problem for some people. Some gluten-containing foods have low FODMAP servings. Also, be aware that some gluten free foods can contain high FODMAP ingredients
Can you eat dairy on the low FODMAP diet?
You can enjoy lots of low lactose or lactose free dairy products on the low FODMAP diet like hard cheeses, lactose free milk or yoghurt, small amounts of sour cream or cream cheese.
Do you need to restart the low FODMAP diet if you have a high FODMAP meal?
No, you don’t. However, you need to make sure you aren’t eating high FODMAP meals all the time; otherwise, you won’t know if the low FODMAP diet is working. Read more about this topic here.
Is the low FODMAP diet sugar free?
The diet isn’t sugar free and you can still enjoy a treat! Types of sugars like white sugar, brown sugar, raw sugar, powdered/icing sugar are all low FODMAP options. Find out what low FODMAP sweeteners you can use here.
How do you deal with constipation on the diet?
The low FODMAP diet can often help reduce bloating and cramps that come with constipation. However, if you choose to do the low FODMAP diet, then it needs to be combined with other food and lifestyle strategies to create a long term constipation management plan. Our dietitian-led Managing Constipation Masterclass in our FODMAP Made Easy Program that will teach you a variety of strategies to help. If you become constipated after starting the low FODMAP diet, you might need to increase the amount of low FODMAP fibre-rich foods and water in your diet (2).
Are alcohol & caffeine allowed during the low FODMAP phase?
There are low FODMAP alcohol and coffee options. However, while on the low FODMAP phase, it is often recommended that you limit your consumption of alcohol and caffeine (1 2). These can be gut irritants and sometimes make gut symptoms worse (1 2). You can test your tolerance to alcohol and caffeine in the reintroduction phase of the low FODMAP diet.
When do you reintroduce high FODMAP foods?
You can start the reintroduction phase after 2 to 6 weeks on the low FODMAP diet (4 5). During the low FODMAP phase, we want to see if reducing the number of high FODMAP foods you are eating has a significant positive impact on your gut symptoms. Of course, we don’t expect your gut to be perfect, but we hope that the low FODMAP diet helps you reduce bloating, excess wind, and altered bowel movements (ideally by at least 50%). If you need help troubleshooting your gut symptoms, join the FODMAP Made Easy program and our team can help.
Once you know how your symptoms have responded, then you can start the reintroduction phase.
Final Thoughts
As you can see the low FODMAP diet is a complex medical diet designed to help people with IBS manage their symptoms. We’re here to make the low FODMAP diet easy with our low FODMAP recipes, free blog articles and FODMAP Made Easy program. Let us know in the comments below what you need help with as you start the FODMAP elimination phase.
Image credit: Alana Scott
References:
1. BPACnz. Irritable bowel syndrome in adults: Not just a gut feeling. Best Practice Journal. 2014: Issue 58. 14-25. Retrieved from http://www.bpac.org.nz/BPJ/2014/February/ibs.aspx
2. Monash University App. About Section & Food Guide. The Monash University Low FODMAP Diet App. 2014: Edition 4. Date retrieved: 2015-03-05. Retrieved from :http://www.med.monash.edu/cecs/gastro/fodmap/iphone-app.html.
3. Nanyakkara, W., Skidmore, P., O’Brien, L., Wilkinson, T., Gearry, R. Efficacy of the low FODMAP diet for treating irritable bowel syndrome. Clinical and Experimental Gastroenterology. 2016-06-17. Doi: 10.2147/CEG.S8798
4. Williams, M. The Low FODMAP Diet for Irritable Bowel Syndrome. Journal for Health Care Professionals. 2014. Retrieved from:http://www.drschaer-institute.com/smartedit/documents/download/dsif_02_2014_us_the_low_fodmap_diet_4.pdf. Retrieved on: 2015-03-09.
5. Monash University. Frequently Asked Questions. Monash University Low FODMAP Website. 2015. Retrieved from:http://www.med.monash.edu/cecs/gastro/fodmap/diet-and-ibs.html#5. Retrieved on: 2015-03-09.
6. Mansueto, P., Seidita, A., D’Alcamo, A., Carroccio, A. Role of FODMAPs in Patients with Irritable Bowel Syndrome: A Review. Nutrition in Clinical Practice Journal. 2015-02-18. DOI: 10.1177/0884533615569886. Retrieved from http://ncp.sagepub.com/content/early/2015/02/17/0884533615569886













Looks like I might finally find help .
Just let us know if you have questions Jo Ann. We’re here to help.
Hello! Thank you for the information C:
I was recommended by my doctor to try the low-fodmaps elimination diet, and I am wondering if this will cause conflict with me being a vegetarian? Will I be able to get enough nutrients without meat or will I need to introduce meat into my diet to get by the elimination phase?
Thank you for any advice <3
Hi Audrey,
It is possible to do the low FODMAP diet while eating vegetarian foods it just might take a bit more planning. Here are a couple of articles that might help:
How to create a balanced vegetarian meal – https://alittlebityummy.com/how-to-create-a-balanced-low-fodmap-vegetarian-meal/
Vegan protein sources – https://alittlebityummy.com/low-fodmap-vegan-protein-sources/
You might also want to check out our Recipe Club which has over 200 vegetarian recipe options (some of these will contain some low FODMAP dairy or eggs): https://alittlebityummy.com/join-our-low-fodmap-club/
Just let me know if you have more questions!
I love this site. Thank you for the hep and information
You are so welcome Susan. Just let us know if there is anything we can do to help you on your journey.
Hi! I am new to all this, I have been diagnosed with IBS and I am not a kitchen person, so the whole idea has me petrified… I don’t know where to start…
Hi Sofia,
We completely understand how overwhelming it can be. First off make sure you grab the Monash University FODMAP Diet App for your food lists. And secondly, if you want more support and to be guided through the 3 phases of the diet then check out our FODMAP Made Easy Program for meal plans, 1200+ low FODMAP recipes, e-courses and more: https://alittlebityummy.com/fodmap-made-easy/
My Dr. Has suggested the FODMAP Diet. I started on Friday. Reading all the articles have helped me follow what to eat. (Recipes as well). How quickly will elimination start or for me to have regular BMs? Thank you.
Hi Cindy,
Everyone reacts differently to the low FODMAP diet. The FODMAP diet helps up to 75% of patients with IBS get good symptom control. How quickly you see changes might depend on a few factors – the type of IBS or gut issue you have, how quickly your remove high FODMAP foods, how good you are at spotting sneaky FODMAPs, and your ability to maintain good fibre intake. If you haven’t seen any positive changes within two weeks of starting the low FODMAP diet, then it will be time to chat to a FODMAP trained dietitian.
Are there certain things/vitamins to help increase fiber intake? Any one specific I should look towards and/ or stay away from?
Hi Joanne,
Thanks for leaving a comment! We have a couple of articles that talk about how to increase your fibre intake while on the low FODMAP diet:
https://alittlebityummy.com/5-low-fodmap-ways-to-boost-your-fibre-intake/
https://alittlebityummy.com/getting-enough-fibre-on-the-low-fodmap-diet/
Looking through the first few recipes, I see ingredients such as mushrooms and onions, which I’ve seen on the “avoid” list from several sources. Could you give further explanation? Thanks!
Hi Susan,
Thanks for commenting. When it comes to mushrooms there are a few low FODMAP options you can try – according to Monash University oyster mushrooms and canned champignon mushrooms are both low FODMAP options that can be enjoyed during the first phase of the diet. For onion replacement, we recommend using the green leaves/tips of spring onion or leek – these green leafy parts are low FODMAP and are a great flavour substitute. You just need to avoid using the white bulbs as this is the high FODMAP part. For an up-to-date list of high and low FODMAP foods we would recommend that you download the Monash University FODMAP Diet App. Additionally, you can find out more about using leeks in low FODMAP meals here: https://alittlebityummy.com/how-to-use-leek-leaves-to-replace-onion-on-low-fodmap-diet/
Hi
I started my elimination phase in January. Yet I still have symptoms. What am I doing it wrong?
Hi Edith,
Thanks for commenting. We are sorry to hear you are still having symptoms. There are multiple reasons why the low FODMAP diet might not work and we talk about those reasons in this article: https://alittlebityummy.com/7-reasons-why-the-low-fodmap-diet-might-not-be-working/
Thank you so much for this site, it’s invaluable. I’ve been on the low FODMAP diet for 10 days and seeing a huge improvement in my symptoms, BUT I have been beating myself up every time I made a mistake and ate something high FODMAP. Thank you for reassuring me that it’s not a calamity and that I haven’t ruined everything! I was worried about going back to my dietitian and having to admit that I’ve failed…
Thanks also for the recipes and tips.
Thank you so much for the lovely comment. It’s great to hear you are finding our resources useful! You definitely won’t ruin everything if you make a mistake so just do the best you can. If you need more help then you might like to check out our FODMAP Made Easy program: https://alittlebityummy.com/fodmap-made-easy/