Have you ever experienced a burning sensation after eating, which spreads up from your stomach into your chest or throat? If you have then you will know what reflux is. This article is going to teach you about what reflux is and give you tips for managing reflux.
Reflux symptoms are uncomfortable and very common, with 15-20% of adults experiencing reflux symptoms at least once every week (1, 2). The good news is that most reflux episodes are mild and quickly resolved. In this article, we’re going to explore what reflux is, the common causes behind reflux, and what you can do about it.
What are the main symptoms of reflux?
The two main symptoms fo reflux often appear as:
- Heartburn – a burning sensation in your throat or chest
- Regurgitation – an acidic taste in your mouth or throat
How does reflux happen?
When you eat, food travels from the mouth to the stomach through a tube called the oesophagus. Where this meets the top of the stomach, there is a circular ring of muscle called the lower oesophageal sphincter (LOS), which relaxes to allow food to pass through. It then closes to prevent the stomach contents from coming back up.
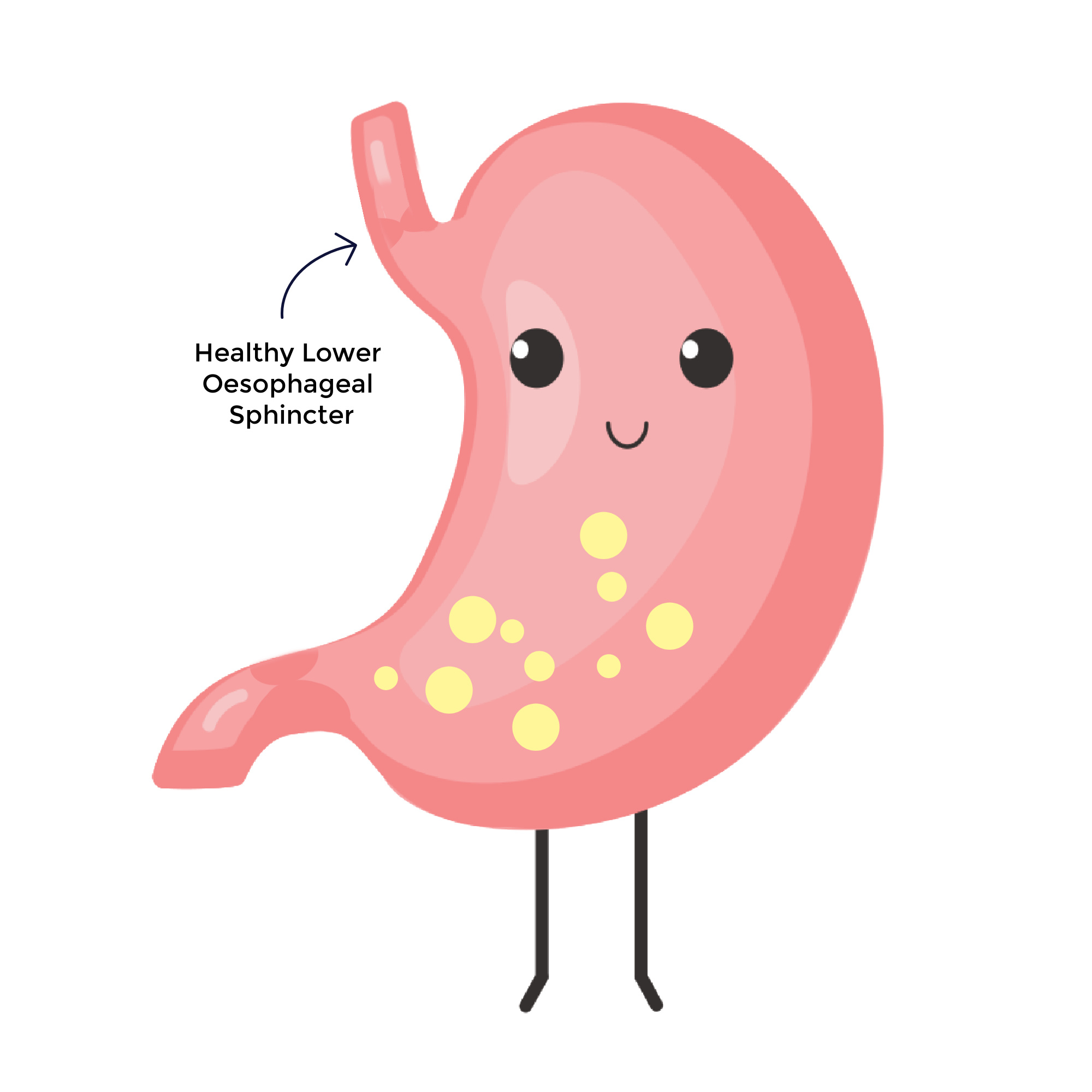
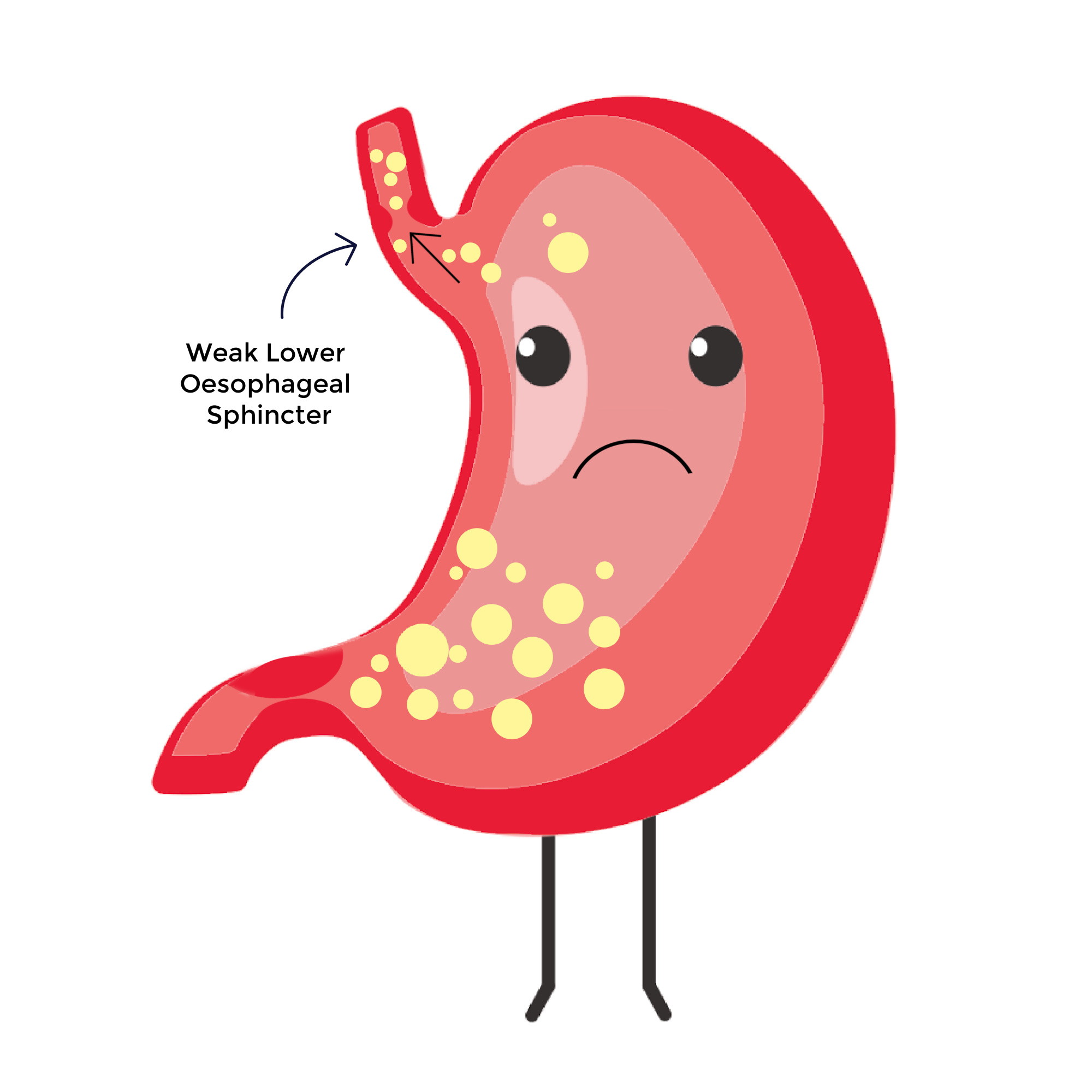
The stomach contains digestive acid which plays a vital role in breaking down our food, and the stomach itself is designed to withstand this acid level. However, when the relaxing and contracting of the LOS doesn’t work properly the stomach acid can come back into the oesophagus, causing “reflux”.
When most people experience reflux it only causes mild symptoms, however gastro-oesophageal reflux disease (GORD) may be diagnosed by a doctor if symptoms become frequent or severe.
What are the common causes of reflux?
Reflux can be caused, or symptoms can feel worse, from a wide range of factors. While this can be frustrating and difficult for people to navigate, it is reassuring that there are a range of dietary and lifestyle factors that can be changed or avoided to reduce reflux.
Dietary Factors For Reflux
It is thought that certain foods may worsen reflux due to the way they work in the body. For example, some foods might relax muscles, decreasing pressure in the LOS or increase acid production.
These include foods such as chocolate, coffee, fatty or fried foods, peppermint, garlic, onion or spicy foods, acid foods (e.g. tomatoes and citrus) and alcohol.
Unfortunately, there is a lot of debate around whether one specific food or food group will cause reflux, so it is important to monitor your own symptoms and food triggers.

Onion & Garlic

Coffee

Fatty or Fried Foods

Chocolate

Peppermint

Spicy Food

Alcohol

Acid Foods
Behavioural Factors Affecting Reflux
As well as food triggers, there are a range of behavioural factors that may contribute to reflux. It’s useful to understand the basics of how digestion works in the body to see if you can reduce your symptoms.
Digestion first begins with seeing, smelling and tasting food. These senses activate a pathway and tells your body to prepare the digestive system for the food. This sends a message to the brain which creates a feedback loop, sending a message back to the stomach to increase stomach acid to help you breakdown the food.
Certain behaviours can reduce your ability to digest food:
- Eating on the go
- Eating in a stressed state
- Eating while distracted

Are you ready to take control of your gut symptoms?
No thanks, my gut is perfect.
Article continues below
Lifestyle Factors Affecting Reflux
These influence general digestion and good health and may increase reflux.

Stress
Stress is known to increase gut symptoms and reduce proper digestion. It is also thought to increase sensitivity to acid and change acid production. (11)

Smoking
As well as the known negative effects of smoking for health, it also reduces saliva production (which neutralises acid in the lower oesophagus). Smoking also lowers pressure in the LOS (making it more relaxed) and increases coughing (which puts more pressure on the LOS). (1-2, 5-6, 12)

Alcohol Intake
Excessive alcohol consumption has many negative health effects, and may also increase reflux due to relaxing the LOS, as well as irritating the oesophagus and stomach lining. (1, 2)

Eating Patterns
Eating patterns such as eating late at night or lying down soon after eating, with symptoms particularly worse following a large high-fat or spicy meal. (3, 5)
Medical Conditions That Can Cause Reflux
1. Hiatus Hernia
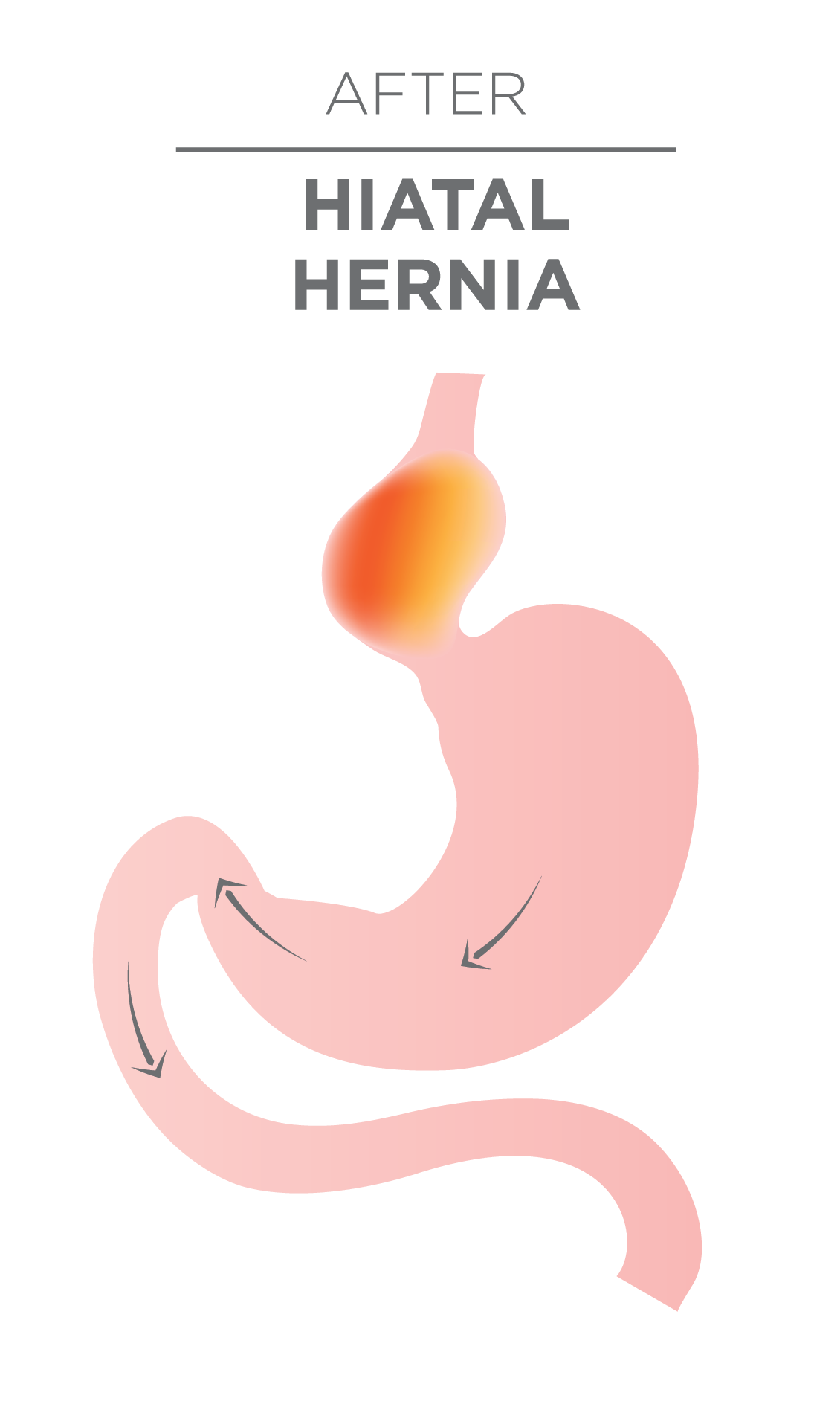
This is where part of the stomach bulges back into the diaphragm. Your diaphragm has a small opening (hiatus) through which your food tube (the esophagus) passes before connecting down to your stomach.
When you have a hiatal hernia, the stomach pushes up through that opening and into your chest. This can allow food and acid to back up into your esophagus, leading to heartburn and reflux. (1)
2. Pregnancy.
Reflux is common in pregnancy as the growing uterus puts pressure on the stomach.
3. Obesity.
The exact mechanism of how obesity causes reflux is unknown, but it may be due to increased pressure on the abdomen. This increased abdominal pressure might also increase the pressure on the LOS enabling reflux to take place.

SUMMARY
What causes reflux? As you can see there is no simple answer. A combination of dietary factors, lifestyle, behavioural and medical factors could be playing a role in your reflux symptoms. Keep reading for strategies that help get rid of reflux.
Strategies To Reduce Reflux
We’re about to get to the nitty-gritty of giving you some practical steps that might help to improve your reflux symptoms. For mild reflux, you can try these tips for managing reflux before seeking medical advice. If your reflux is severe or you have been getting it for a while, then please go and see your doctor. Your doctor might recommend medication to help, along with the strategies we discuss below.
Lifestyle & Behavioural Strategies
That Reduce Reflux

Eating Habits
- Take your time to eat – eat slowly and chew food carefully
- Avoid large meals and do not overeat at one time
- Stay upright for at least 20 minutes after eating
- Avoid eating late at night (5) – try to leave at least 2 hours after eating before going to bed
Sleeping Habits
Elevate the head of your bed for sleeping, adding a foam wedge under your mattress or wooden blocks under the legs of the bed (1, 5, 13)


Lifestyle Habits
- Avoid wearing tight fitting clothes (1)
- Maintain a healthy weight
- Incorporate light, gentle exercise
- Stop smoking
Stress Management Habits
Include mindfulness, stress management strategies or relaxation techniques, such as breathing exercises (11, 14)
Dietary Changes That Help Reduce Reflux
Since everyone is different, it is important to monitor your own reflux symptoms and avoid any foods or drinks which make your symptoms worse. Trigger foods and tolerance levels will differ for everyone, so it may be useful to work with a dietitian for this. Common advice includes:

Choose small, frequent meals, rather than large portions at one time.

Eat a fibre-rich diet, increasing intake of non-citrus fruits, vegetables, wholegrains and legumes (16).

Include a wide range of vegetables, choose non-citrus fruits such as strawberries or just ripe bananas.

Choose wholegrains such as oats, wholegrain rice and quinoa.

Reduce carbonated or fizzy drinks (4, 6) and caffeinated drinks such as coffee and tea (15)

Reduce saturated fats, opting for healthy fats such as olive oil, avocado, nuts and flaxseeds

Trial reducing common trigger foods such as high fat foods, spicy or acidic foods, garlic, onion and chocolate

Moderate or limit alcohol intake
Beyond Dietary and Lifestyle Changes
For many people the above tips for managing reflux can help them control their symptoms, however it is also important to know when to seek help.
It’s time to see your doctor if symptoms are severe, if you are unable to control them or if they have lasted for many years. This is important as long-term exposure to acid in the oesophagus can cause significant damage over time (3). The medical treatment you receive will be based on how frequent or severe your symptoms are.
You must also see your doctor immediately if you are having any “red flags”, including difficulty or painful swallowing, vomiting blood, chest pain or unintentional weight loss (1). A doctor will then do further tests to rule out other medical problems that may have similar symptoms to GORD.
Medications
There are a range of medications that can help with reflux, which work by reducing or stopping the production of stomach acid. These include antacids, surface agents, histamine blockers or proton pump inhibitors. Most people are familiar with antacids, such as Mylanta or Gaviscon, as these are available without prescription.
Before you start taking any medication for your reflux, it is important to talk to your GP or doctor about which is right for you. Please also take these medications only as advised, as being on these medications long term can have other effects. These effects may include reducing the absorption of certain nutrients such as iron, calcium and vitamin B12 (17), and increase the risk of bacterial infection (18) or small intestinal bacterial overgrowth (19).
Where Does The Low FODMAP Diet Fit?
Reflux can occur alongside other gut conditions like IBS. So what happens if you are following the low FODMAP diet for your IBS and have reflux as well?
The low FODMAP diet can be used along with the reflux strategies we’ve talked about so let’s look at the similarities and differences between the diets.
Similarities
It is important for everyone, whether those on a low-FODMAP diet or those with reflux, to make a conscious effort to take time eating meals, eating slowly and chewing food well.
This simple change is crucial for proper digestion of food, and can result in a significant improvement in a range of gut symptoms.
Stress management strategies and mindfulness can be helpful for both conditions as well.
Avoiding smoking and limiting excessive alcohol should also be first-line factors to consider before any dietary changes are made, as these will exacerbate any reflux or other gut symptoms.
Eating regular meals throughout the day is important for both low-FODMAP diets and preventing reflux. Eating a large portion at one time, which is often the result of not eating enough during the day, puts a large amount of pressure on the gut and subsequent negative symptoms.
As well as being high-FODMAP, garlic and onion are acidic foods which can irritate the oesophagus, so may be beneficial to be avoided for both conditions.
Differences
There are certain foods which are low-FODMAP which may trigger reflux symptoms.
Our favourite low FODMAP go-to peppermint is one of them!
While peppermint products, including peppermint tea, can be helpful with IBS-symptoms, these are known to relax the LOS and can increase reflux.
Foods such as dark chocolate and acidic but low FODMAP foods (oranges, lemons, limes, pineapples and tomatoes) may irritate the oesophagus or cause reflux. Instead choose fruit like firm bananas (no brown spots), strawberries, and rockmelon – these fruits all have small low FODMAP serving sizes.
But remember – everyone is individual –so if you have been happily having an orange or peppermint tea with no reflux – you can continue to have it!
Increasing fibre content is recommended to help reduce reflux symptoms (16), however this can be difficult in the restrictive phase of the low-FODMAP diet. Check out our tips for increasing fibre here.
While on the low-FODMAP phase, it is important to avoid “stacking” too many fruits or vegetables at one time. Focus on spacing your fruit serves 3 to 4 hours apart and creating a balanced meal. A balance meal contains a serve of protein, a carb like potato, rice quinoa, gluten free pasta, and 1/2 plate of vegetables (choose 2 or 3 different low FODMAP options).
SUMMARY
Hopefully this article has helped you understand what causes reflux and provided you with lots of tips for managing reflux. Your next step is to talk to your health care provider about dietary, lifestyle, and medical factors that might be contributing to your reflux before you consider what treatment options might be right for you.











Leave a Reply